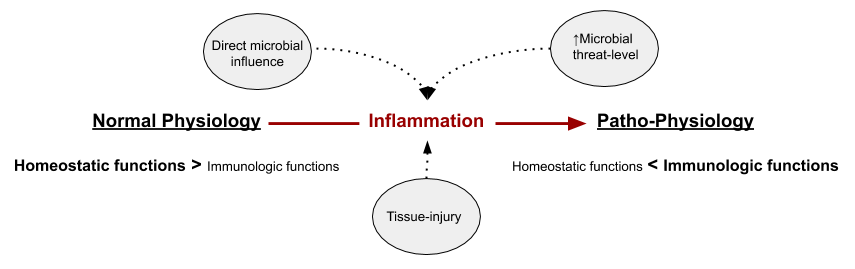
Inflammation is a process orchestrated by a complex interplay between several cell-types with the common goal of removing unwanted cells and substances of both domestic and foreign origin, and to enable efficient repair in the case of injury. Activation of the inflammatory response necessitates a temporary compromise between the energetics of parenchymal cells and non-parenchymal cells because resources needs to be directed towards processes carried out by the later, such as tissue-repair and microbial defence. It’s a necessary response to injury and infection, being greatly amplified if the two co-occurs. Normally inflammation has a transient nature, and it only poses a problem if the stimulus is persistent or cyclic which puts the affected tissues in a state of pseudo-starvation over time, leading to progressive loss-of-function and degeneration. Stimulation of tissue parenchymal cells with pro-inflammatory cytokines from leukocytes commonly results in those cells adopting an insulin-resistant phenotype, which includes up-regulated autophagy, lowered oxidative metabolism and increased levels of reactive oxygen species (ROS).
Supporting Evidence
- Inflammation is a response to cellular stress, and is antagonistic to homeostatic control mechanisms.1)https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3601794/
- Inflammation mainly takes place in the ECM.2) … Continue reading
Association with Disease
- Increased levels of inflammatory cytokines in MA, OA, DDD/DH, RA, TP and AS.3)https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5328896/4)https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6780543/5)https://www.ncbi.nlm.nih.gov/pubmed/97432156)https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7006114/7)https://www.ncbi.nlm.nih.gov/pubmed/9222884
References